Diagnose 4
- Gewebestörung an der Augenoberfläche
=> hier finden Sie eine vereinfachte Übersicht Diagnostischer Verfahren für das Trockene Auge
Epithel Zustand
Hauptursachen für Epithelstörungen und Oberflächenschädigung
Epithelstörungen treten auf, wenn die normale Gesundheit der Augenoberfläche in einem Ausmass eingeschränkt wird, dass zu Symptomen führt. Epithelstörungen entstehen durch zwei Hauptursachen, nämlich
durch erhöhte mechanische Reibung bei Trockenheit, durch den Mangel an ´Schmiermittel´ zwischen Augapfel und Augenlidern, und
durch erhöhte Osmolarität (Hyperosmolarität), bei erhöhter Konzentration der Salze und Proteine in den Tränen, wenn das Tränenwasser bei Ölmangel zu schnell verdunstet.
Chronische mechanische Reibung und Hyperosmolarität erscheinen derzeit als die wichtigsten sekundären pathogenetischen Faktoren aufgrund von Tränenfilmstörungen. Oberflächenschäden, beginnend mit dem Epithel, induzieren eine Abfolge von sekundären pathogenetischen Faktoren, die zu entzündlichen Reaktionen führen. In chronischen Stadien kann dies zu einer chronischen Beschädigung des Gewebes der Augenoberfläche bei schwerem Trockenen Auge führen. Diese Pathophysiologie des Trockenen Auges wird in der Animation zum Holistischen Dynamischen Konzept der Pathophysiologie des Trockenen Auges dargestellt
Bei Betrachtung der Pathophysiologie wird das Trockene Auge leichter verständlich
Obwohl chronische mechanische Reibung und hyper-Osmolarität wichtige Faktoren sind beim Trockenen Auge, handelt es sich doch, in pathophysiologischer Sicht, nicht um primären Ereignisse.
Sie entstehen erst sekundär, nämlich aufgrund von anderen vorhergehenden primären Ereignissen, typischerweise der Tränenfilm-Störung … und diese wiederum beruht auf den grundlegenden kausalen Faktoren wie Störungen der Tränenbildung (durch die Drüsen) und Störungen der Ausziehung der Tränen zu einemdünnen aber stabilen Tränenfilm beim Lidschlag.
Deutlich seltener im üblichen Patientengut kann zuerst ein primärer Gewebeschaden auf treten, durch innere oder äussere schädliche Risikofaktoren.
Die pathophysiologische Sichtweise ist ein Ansatz zum Verständnis der ursächlichen Zusammenhänge einer Erkrankung und ist damit eine Basis zur Ermittlung erfolgreicher Therapieansätze.
Dies ist der Grund, warum sich das neue Holistische Dynamische Konzept des Trockenen Auges streng nach dem pathophysiologischen Verlauf richtet ... denn auch die Meinung über Faktoren, die heute als wichtig angesehen werden kann sich möglicherweise schon morgen verändern.
Reibung und Hyperosmolarität - 2 wichtige Sekundäre Pathogenetische Faktoren
mechanische Reibung
Erhöhte mechanische Reibung ist ein hauptsächlicher pathogenetischer Faktor für Augenoberflächenerkrankungen. Reibung tritt bei allen Bewegungen des Augapfels relativ zur knöchernen Orbita und zu den Augenlidern auf, insbesondere beim Lidschlag. Pathologisch erhöhte Reibung tritt auf wenn die normale Schmierung durch den Tränenfilm aufgrund der Pathologie z. B. beim Trockenen Auge oder aufgrund äusserer Faktoren wie einer Kontaktlinse verringert wird.
mechanische Reibung ist ein wichtiger (sekundärer) pathogenetischer Faktor
entsteht unvermeidlich zwischen der Schleimhaut der Bulbus (Hornhaut und bulbäre Konjunktiva) und der palpebralen Konjunktiva der Augenlider
tritt zwangsläufig bei Augenbewegungen und beim Lidschlag auf
wird durch natürliche Schmiersysteme/ Lubrikations-Systeme der gesunden Augenoberfläche begrenzt, um Gewebeschädigung zu vermeiden.
erhöhte Reibung kann Schäden und Entzündung auslösen
entsteht durch zusätzliche Risikofaktoren wie z.B.
Mangel an Tränenwasser, wie z. B.
beim Trockenen Auge durch austrocknende Umweltfaktoren (Evaporatives Trockenes Auge), oder
bei wässrigem Tränenmangel (Tränen-defizientes Trockenes Auge) bei Störungen der Tränendrüse, z.B. beim seltenen Sjögren-Syndrom
Mangel an Muzinen aufgrund chronischer Oberflächenschäden
zusätzliche äußere Faktoren wie z. B. eine Kontaktlinse, die zu einer Augentrockenheit führen oder diese verstärken kann
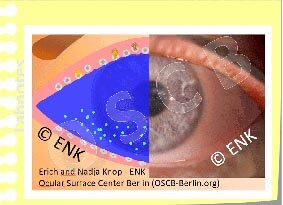
Die schematische Darstellung zeigt den Einfluss einer lokalen Hyperosmolarität, durch Verdunstung von Tränenwasser mit Ansammlung der verbleibenden Tränensalze und Proteine (graue Kreise) und lokalem Aufbrechen des Tränenfilms. Die Hyperosmolarität zieht Wasser aus den Epithelzellen mit potentieller Schrumpfung und Zellbeschädigung. Dies stellt ein Gefahrensignal dar und löst eine Entzündungsreaktion mit Bildung von Entzündungsmediatoren aus. Bei chronischer Tränenfilmstörung mit Hyperosmolarität kann sich ein entzündungsförderndes Milieu bilden, das zum Ausbruch oder zur Verschlimmerung eines chronischen trockenen Auges führen kann. (Aus schematischen Gründen ist die lokale Hyperosmolaritätszone hier viel zu klein - es kann davon ausgegangen werden, dass auch eine kleine lokale Hyperosmolarität bereits mehrere oder viele Zellen gleichzeitig beeinflusst).
Hyperosmolarität des Tränenfilms ist ein weiterer wichtiger (sekundärer) Faktor
eine ungewöhnlich starke Erhöhung der Osmolarität der Tränenflüssigkeit über den Normalwert von knapp 300mosm / l (Milliosmol pro Liter)
typischerweise durch vermehrte Verdunstung von wässrigen Tränen
aufgrund eines Mangels an Tränenfilml-Lipiden
meist bei obstruktiver Meibom-Drüsen-Dysfunktion (MGD)
oder bei niedriger Lidschlagfrequenz mit geringer Abgabe von Lipiden aus den Drüsen
bei zusätzlichen Risikofaktoren, wie trockener Umgebung oder Kontaktlinsen
durch Verdunstung des Tränenwassers kommt es zur Konzentration von Salzen und osmotisch aktiven funktionellen Proteinen in der verbleibenden geringeren Tränenmenge
es kann dann zumindest lokal zu Hyperosmolarität vorkommen
die eine hyperosmolare Belastung auf das Epithel ausübt
indem den Epithelzellen Wasser entzogen wird, was zur Entstehung von Oberflächenschäden und Aktivierung einer Entzündungsreaktion führen kann - symptomatisch wird oft das Augenbrennen auf eine erhöhte Osmolarität zurückgeführt.
Erhöhte Reibung und erhöhte Osmolarität sind die beiden wichtigsten sekundären pathogenetischen Einflussfaktoren für das Auftreten von epithelialen Defekten und weiterer nachfolgender Oberflächenschädigung, oft durch Entzündung.
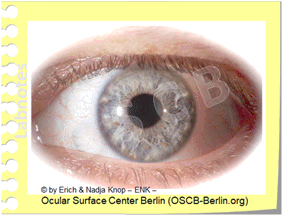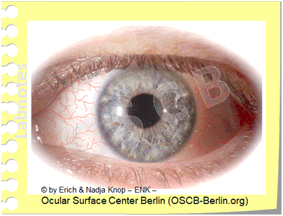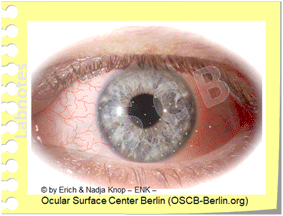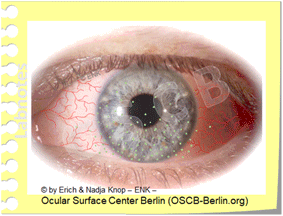
Zonen erhöhter mechanischer Reibung beim Trockenen Auge
Reibung tritt hauptsächlich an der Bulbusoberfläche innerhalb der Lidspalte und am hinteren Rand der Augenlider auf, hauptsächlich im oberen Augenlid. Unter normalen Bedingungen steht ausreichend ´Schmierung´ durch eine ausreichende Menge von Tränenflüssigkeit und zusätzliche lubrikative Substanzen zur Verfügung. Unter Bedingungen erhöhter Reibung, wie z.B. beim Trockenen Auge oder beim Tragen von Kontaktlinsen, können die normalen Bewegungen von Augapfel und Lidern gegeneinander bereits Epithelschäden verursachen. Dies kann durch 'Vitalfärbung' mit verschiedenen Farbstoffen sichtbar gemacht werden, da die verletzten Zellen die Färbung aufnehmen und die normalen nicht. Die Vitalfärbung der erhabenen Epithellippe der ´Lid Wiper´ (Lidwischer) an der hinteren Lidkante wird von Donald KORB und Kollegen als Lid Wiper Epitheliopathy (LWE) bezeichnet.
an der Bulbus-Oberfläche
an der hinteren Lidkante (´Lid Wiper´)
an der hinteren Lidkante, wo die Reibungskräfte des Oberlids durch Auflage auf dem Bulbus konzentriert sind. Es wurde beobachtet, dass die Lid Wiper Epitheliopathie (LWE) mit pathologischer Vitalfärbung der empfindlichste Indikator für eine erhöhte Reibung an der Augenoberfläche ist.
Diese kleine Sammlung der wichtigsten pathogenetischen Faktoren beinhaltet noch keine schwerwiegenderen Veränderungen des äußeren Milieus, z.B. bei Verätzungen der Augen durch aggressive Chemikalien oder nach allen Arten von Unfällen oder schweren Infektionen, die vorkommen können, aber weniger häufig sind als chronische mechanische Reibung und lokale Hyperosmolarität.
Vitale Anfärbung
Eine schematische Zeichnung zeigt das Bild von Fluorescein-gefärbten Epithelveränderungen, die als kleine Punkte auftreten. Die Größe der gefärbten Punkte, die prinzipiell von einzelnen gefärbten Zellen stammen, ist hier in der Zeichnung etwas zu groß, um sie besser sichtbar zu machen. Spezifische Färbungsmuster können wie hier bandförmig innerhalb der Lidspalte auftreten. Färbungsmuster können jeweils Vermutungen zum Mechanismus der pathologischen Veränderung zulassen.
Die Darstellung von Beschädigungen der Augenoberfläche durch Vitalfarbstoffe ist ein etablierter Eckpfeiler in der Diagnostik der Augenoberfläche generell und speziell beim Trockenen Auge.
Verschiedene Farbstoffe (z.B. meistens Fluoreszein, seltener Lissamingrün) werden in der Klinik direkt auf das lebende vitale Gewebe gegeben. Die Farbstoffe richten keinen Schaden an - ausser gelegentlich einer gewissen Irritation bei Bengalrosa. Da diese Farbstoffe topisch an der Augenoberfläche sind, werden sie gelegentlich auch als ´Topische Farbstoffe´ bezeichnet.
Die Bezeichnung als ´Vitalfarbstoff´ steht in Kontrast zu ´Histologischen Farbstoffen´, die im Labor auf fixierte und daher tote Zellen gegeben werden. Der Begriff ´Vital´ bezieht sich auf die gefärbten Zellen und nicht auf den Farbstoff selbst, da einige Farbstoffe sowohl bei vitalem Gewebe als auch bei fixiertem Gewebe angewendet werden - dies betrifft z.B. Lissamingrün.
Eine schematische Zeichnung auf zellulärer Ebene zeigt das Bild von mit Fluoreszein-gefärbten epithelialen Veränderungen, die als kleine Punkte auftreten. Die gefärbten Punkte, stammen prinzipiell von einzelnen gefärbten Zellen und sind hier als polyedrische Objekte dargestellt. Oft betrifft dies mehr als eine einzelne Zelle, so dass die gefärbten Flecken größer als ein Zelldurchmesser sind.
Vitalfärbung Prinzip
Das Färbeprinzip besteht darin, dass die Bindung von Substanzen durch intaktes Gewebe typischerweise gehemmt ist und gleich weggespült wird durch die Tränen.
Daher werden nur Bereiche der Augenoberfläche sichtbar gemacht, deren normale Integrität in irgendeiner Weise verändert ist.
Die Oberflächenveränderung/ Oberflächenschaden kann entweder auf zellulärer Ebene durch Beschädigung der Zellmembran oder (nur) auf der Ebene des extrazellulären Muzins durch Veränderung oder Entfernung der Muzine erfolgen. Vitalfärbungen treten typischerweise in Form von kleinen Punkten auf, die nur durch Vergrößerung in einer Spaltlampe erkennbar sind.
Die Schwere der Augenoberflächenfärbung , die aufgrund pathologischer epithelialer Veränderungen auftritt, wird typischerweise gemäß der Menge der gefärbten Zellen bestimmt. Die Stelle scheint auch eine gewisse Bedeutung zu haben, da die Nasenfärbung (oberes Bild) typischerweise mild und unspezifisch ist, wohingegen die zeitliche Färbung (unteres Bild), dh an einer Stelle, an der die frischen Tränen aus den Tränendrüsenausscheidungen typischerweise in den Bindehautsack fließen deutet auf eine schwerere Erkrankung hin und ist etwas spezifisch für die Erkrankung des trockenen Auges (Schematische Darstellungen gemäß Beobachtungen von UCHIYAMA und Kollegen 2009 ).
Vitalfärbung Konzept
Das allgemeine Konzept ist, dass eine erhöhte Färbung einer erhöhten Schädigung entspricht und somit einer erhöhten Schwere der Erkrankung.
Wie in den Kapiteln über die "Grundlegenden funktionellen Komplexe" der Augenoberfläche und über “Grundlegende kausale Faktoren“ des Trockenen Auges erläutert, sind die pathologischen Veränderungen des Epithels typischerweise negative Auswirkungen der Tränenfilmstörung.
Selten kann aber auch das Gewebe zuerst geschädigt sein und dadurch die Stabilität des Tränenfilms stören
Gewebeschäden treten vor allem auf durch die sekundären pathogenetischen Faktoren von: chronisch mechanischer Reibung und chemischer Irritation durch einen hyperosmolaren Tränenfilm, aufgrund erhöhter Verdunstung von wässrigen Tränen.
Vitalfärbung Ort
Man darf annehmen, dass die Oberflächenschädigung bei Tränenfilmstörungen vor allem im Bereich der geöffneten Lidspalte auftritt. Dort ist das Gewebe der Luft ausgesetzt wenn die Augenlider zum Sehen geöffnet sind.
Die Anfärbung tritt daher vor allem an der Kornea und an der bulbären Konjunktiva auf. Allerdings kann schädliche mechanische Reibung auch an den hinteren Lidkanten, vor allem beim Oberlid auftreten, durch die Reibung auf dem Bulbus beim Lidschlag.
Ausserdem wurde beobachtet, dass an der bulbären Konjunktiva die meiste Färbung dort auftritt, wo sich am wenigsten Tränenflüssigkeit befindet. Da die Tränenflüssigkeit von temporal in den Bindehautsack eintritt, ist es dort im interpalpebralen Spalt bereits physiologisch feuchter als nasal.
Eine Anfärbung nasal kann daher leichter einmal auftreten. Eine temporale Anfärbung, wo es physiologisch ´feuchter´ sein sollte, gilt daher als spezifischer für eine Tränenfilmstörung bei Trockenem Auge als eine nasale Anfärbung (McCULLEY und Kollegen im Ophthalmology Newsmagazine 2008).
Vitalfärbung - Quantifizierung - Oxford SCORE
Die VITALFÄRBUNG von epithelialen Veränderungen der Augenoberfläche wird beispielsweise semiquantitativ bewertet, wobei die Menge der Färbung den einzelnen gefärbten Zellen entspricht, durch Vergleich mit einer Tabelle, der bestimmten Modellgrade anzeigt, abgeschätzt wird. Ein beliebtes Bewertungssystem ist der OXFORD SCORE, da dieser einfach zu verwenden ist und relativ zuverlässige Ergebnisse liefert. Die hier gezeigten Färbungsintensität stellt schematisch eine mittlere (Grad 2) Färbung auf der Oxford-Skala dar.
Die Menge und oft auch die Verteilung der Färbung wird nach verschiedenen Bewertungssystemen eingeschätzt, von denen der OXFORD-Score wahrscheinlich am häufigsten verwendet wird.
Der Oxford Score erfasst die Intensität der Färbung, d.h. die Menge der gefärbten Punkte, getrennt für die nasale und temporale Bindehaut und für die Hornhaut. Die Stärke der Färbung wird dann in sechs Stufen mit zunehmender Stärke von 0 bis 5 bewertet.
Die Bewertung erfolgt in semi-quantitativer Weise durch Vergleich der Färbung eines einzelnen Patienten mit den sechs Bewertungsdiagrammen, die eine Darstellung der verschiedenen Färbebilder zeigt. Dieses System ist relativ zuverlässig und wird häufig für wissenschaftliche Studien verwendet.
Disparität von klinischen Befunden und Symptome beim Trockenen Auge
Die Bestimmung der Stärke der Vitalfärbung erlaubt eine gute klinische Einschätzung der Oberflächenstörung und damit im Prinzip meist auch des Schweregrades eines Trockenen Auges.
Allerdings ist dies noch nicht die ´ganze Wahrheit´, denn die Erkrankung des Chronischen Trockenen Auges ist ein komplexes Krankheitsbild, in dem klinische Befunde nicht immer mit dem subjektiven Krankheitsgefühl des Patienten übereinstimmen. Dies liegt unter anderem daran, dass sich beim Trockenen Auge komplexe Störungen des Schmerzsystems auf verschiedenen entwickeln können (neuropathischer Schmerz).
Es kann sich ein Schmerzsyndrom entwickeln, das auch bei klinische moderatem oder leichten Befund besteht oder das weiterbesteht trotz klinischer Befundbesserung eines Trockenen Auges. Eine Zusammenarbeit mit der Schmerzmedizin, Psychosomatik und auch Neurologie, kann hier hilfreich sein,
Palpebrale Epitheldefekte - Vitalfärbung - Lid Wiper Epitheliopathy (LWE)
Mechanishe Reibung tritt hauptsächlich an der Bulbus-Oberfläche innerhalb der Lidspalte und an der hinteren Lidkante auf, hauptsächlich im oberen Augenlid, aber bis zu einem gewissen Grad auch im unteren Lid. Die verdickte Epithellippe des Lidwischers. Sie reicht am hinteren Rand bis zu ca. 10 mm nach innen und die Region des Augenlides, die in Kontakt mit dem Bulbus ist. Die auftretende Reibungskraft beim Lidschlag konzentriert sich hier auf eine relativ kleine Fläche. Normalerweise wird die Reibung durch ein ausreichendes Tränenvolumen und ein reichhaltiges Muzin-Wasser-Gel durch viele Becherzellen und Becherzellkrypten (siehe 2 Abbildungen rechts), ausreichend begrenzt. Bei erhöhter Reibung, wie beim Trockenen Auge und bei Kontaktlinsentragen, tritt eine pathologisch hohe mechanische Reibung und damit Veränderung und Verwundung des Epithels am Lidwischer auf. Lid Wiper Epitheliopathy (LWE) ist das erste und empfindlichste Zeichen für erhöhte Mechanische Reibung an der Augenoberfläche (KORB und Kollegen 2000).
Reibung tritt auch am palpebralen hinteren Lidrand auf
Bei erhöhter Reibung an der Augenoberfläche, wie z.B. beim Trockenen Auge und beim Tragen von Kontaktlinsen, kann es auch zu Schäden an der hinteren Augenlidkante kommen, die durch Vitalfärbung sichtbar gemacht werden können.
Dies betrifft insbesondere die marginale Bindehaut an der palpebralen Seite des hinteren Lidrandes, den LID WIPER (Lidwischer). Diese Zone befindet sich in unmittelbarer Nähe zum Bulbus, während der Rest der tarsalen Konjunktiva durch den schmalen Tränensee des "Kessing´s Space" vom Augapfel getrennt ist.
Die erhöhte Epithellippe des Lidwischers ist der Teil des Augenlides, der während eines Lidschlages über die Bulbusoberfläche wischt. Der Lid Wiper komprimiert beim Lidschluss den ´alten´ Tränenfilm, der häufig schon dünne Bereiche oder sogar Störungen aufweist, beim Absenken des oberen Augenlides. Während des Aufwärtshubs des Lides verteilt der Lidwischer einen neuen Tränenfilm (siehe Animation unten).
Die Reibungskräfte während des Lidschlages konzentrieren sich auf den Lidwischer
Daher ruhen die meisten oder fast alle Reibungskräfte des Augenlides auf der Lidwischerzone. Unter Bedingungen mit erhöhter Reibung an der Augenoberfläche ist der Lidwischer folglich die Zone, in der die meisten Veränderungen und Verwundungen auftreten.
Tatsächlich wurde von KORB und Kollegen in mehreren Berichten als ein sehr empfindlicher erster Indikator für erhöhte Reibung bei Patienten mit trockenem Auge und bei Kontaktlinsenträgern über eine lebenswichtige epitheliale Färbung der Lidwischerzone berichtet, die als Lidwischer Epithelipathie bezeichnet und als LWE abgekürzt (Abbildung).
LWE trat bereits dann auf, wenn herkömmliche Marker für trockene Augen, wie die kurze Auflösungszeit für Tränenfilme (BUT) oder der Schirmer-Test, noch normal oder grenzwertig normal waren. Patienten mit einer Krankheit des trockenen Auges, die entsprechende Symptome umfasst, haben überwiegend (ungefähr vier Fünftel) LWE, wohingegen Patienten ohne entsprechende Symptome des trockenen Auges nur selten LWE von irgendeinem Grad haben. LEW ist daher ein wichtiger und sehr spezifischer Indikator für erhöhte mechanische Reibung an der Augenoberfläche.
Die Einstufung der Lidwischer- Epitheliopathie richtet sich nach der Ausdehnung der Veränderungen
Der Schweregrad von LWE wird gemäß der Ausdehnung der Vitalfärbung in zwei Dimensionen - vertikale Höhe und horizontale Breite - in 4 Stufen von 0 bis 3 eingestuft, wie von KORB und Kollegen 2010 im Cornea Journal erläutert :
Die vertikale Höhe wird wie folgt eingestuft:
in Teilen der LW-Höhe
25% 0 (normal)
25% bis 50% 1 (mild)
50% bis 75% 2 (mäßig)
75% 3 (schwer)
Die horizontale Breite wird wie folgt eingestuft:
<2 mm 0 (normal)
2–4 mm 1 (mild)
5–9 mm 2 (mäßig)
> 10 mm 3 (schwer)
Der Mittelwert für beide Dimensionen bildet die Gesamtnote von LWE.
OPTIMALE VITALFÄRBUNG von LWE
LWE-Färbungen mit allen hier behandelten gewöhnlichen Chromophoren - Fluorescein, Lissamine Green und Rose Bengal.
Die Intensität der Vitalfärbung kann durch Mischen von 2% Fluorescein mit 1% Lissamingrün und zweimaliges Auftragen eines Tropfens (40 µl) pro Auge im Abstand von 5 Minuten optimiert werden. Die Färbung kann eine Minute nach dem zweiten Tropfen analysiert werden.
Verschiedene Vitalfarbstoffe
Es gibt verschiedene Vitalfarbstoffe, die häufig austauschbar verwendet werden, obwohl sie leicht unterschiedliche Färbeprinzipien haben.
FLUORESCEIN Vitalfärbung des L id Wiper Epitheliu m des marginalen Konjunktiva. Die Färbung ist intensiv blaugrün. Fluorescein färbt die pathologische Lid Wiper Epitheliopathie (LWE), liegt aber auch auf der Tarsal Conjunctiva in der Mitte des Bildes und grenzt teilweise Substrukturen wie Krypten und andere Oberflächenunregelmäßigkeiten ab. Diese Überlagerung von Fluorescein auf dem Epithel ist keine echte Färbung, da, wie im nächsten Bild mit Lissamine Green-Färbung zu sehen ist, die Tarsalkonjunktiva bei solchen Patienten typischerweise unverändert und gesund ist.
FLUORESCEIN:
In der ophthalmologischen Praxis am häufigsten verwendet wird wahrscheinlich Fluorescein, ein fluoreszierendes Molekül mit bläulich-grüner Farbe in der Spaltlampe. Ein großer Vorteil ist sicherlich, dass Fluorescein ein Mehrzweckfarbstoff ist , der verwendet werden kann:
zur Beobachtung der Unversehrtheit der Augenoberfläche im Hinblick auf epitheliale Veränderungen - oft einfach als " Vitalfärbung " bezeichnet
Fluorescein eignet sich besser zur Untersuchung von Hornhautveränderungen, wohingegen die Bindehaut , die ebenfalls unter der Pathologie leidet, z. B. bei trockenem Auge, schwächer färbt
Die Sichtbarkeit von Fluorescein kann jedoch durch die Verwendung spezifischer Filter zur Anregung (blau) und zur Beobachtung (orange) verbessert werden.
zur Beobachtung der Tränenfilmintegrität im Fluorescent Break-Up Time Test ( F- ABER)
zur Unterstützung beim Anpassen von Kontaktlinsen ... was für RGP jedoch am sichersten ist, da weiche Hydrogel-Linsen den Fleck auffangen können
zur leichteren Beobachtung der Tränenmeniskushöhe (TMH) ... wenn sichergestellt ist, dass das aufgebrachte Volumen klein genug ist, um eine fehlerhafte Ablesung eines hohen TMH zu vermeiden, obwohl dieser tatsächlich niedrig ist
Ein dreifacher Ansatz ist mit flUOrescein möglich :
Da Fluorescein sowohl EPITHELIAL ALTERATIONS als auch TEAR FILM färbt , kann es für verschiedene Untersuchungen verwendet werden:
zunächst für Auswertung des Tränenfilms mit Bezug auf B REAK- U P T IME ( BUT ) und
Tear MENISCUS Height (TMH) und danach, wenn Fluorescein einige Minuten eingetaucht ist, typischerweise 5 Minuten, kann es für verwendet werden
Bewertung von Epithelveränderungen ' Vitalfärbung '
... dies ist ein zeitsparender praktischer Ansatz in Augenkliniken.
Lissamingrün Vitalfärbung des L id Wiper Epitheliu m des marginalen Konjunktiva. Die Färbung ist intensiv dunkelgrün und färbt die Bindehaut sehr gut und intensiv. Hier macht es die pathologische Lid Wiper Epitheliopathy (LWE) sichtbar, da die Bindehautzellen, die sich bei erhöhten Reibungszuständen wie Augentrockenheit und Kontaktlinsenabnutzung verändern, den Fleck aufnehmen, wohingegen die anderen normalen Bindehautzellen an der Tarsal Conjunctiva in Die Bildmitte färbt nicht.
LISSAMIN GRÜN
Lissamin färbt sich, wie der Name schon sagt, grün und bindet an veränderte und abgestorbene Zellen, z. B. bei Erkrankungen des trockenen Auges
Es färbt die Bindehaut besser als Fluorescein
Für die Tränenfilmanalyse ist Lissamingrün wenig geeignet und daher grundsätzlich auf Zellveränderungen beschränkt
Bengalrosa Vitalfärbung des L id Wiper Epitheliu m des marginalen Konjunktiva. Die Färbung ist intensiv rötlich-rosa . Die lebenswichtige Färbung des Lidwischers ist pathologisch und wird als Lidwischer-Epitheliopathie (LID Wiper Epitheliopathy, LWE) bezeichnet, wohingegen die Färbung der dünnen Linie (Pfeile) an der Außenseite normal ist und die physiologisch färbbare L ine von MAR X anzeigt .
ROSE BENGAL
Rose Bengal hat eine rötliche bis rosafarbene Farbe und ist den Patienten wahrscheinlich am besten bekannt, da ihre topische Anwendung zu einem ausgeprägten Stechgefühl führt
Es hat ein ähnliches Färbespektrum wie Lissamingrün, ist also besser für Bindehautveränderungen geeignet
Im Gegensatz zu Lissamin färbt Rose Bengal neben veränderten auch Muzine und gesunde Zellen, wenn sie aufgrund von Lücken in der Muzinschicht Zugang zu gesunden Zellen haben. Diese Eigenschaften können die Interpretation der Rose Bengal-Färbung im Vergleich zu Lissamingrün und Fluorescein etwas erschweren.
Zusammenfassung Vital Stains:
Fluorescein ist der entscheidende Mehrzweckfarbstoff für die Augenoberfläche und den Tränenfilm, während Lissamine Green für die Untersuchung der Bindehaut vorzuziehen ist, da es Bindehautveränderungen stärker färbt. Aufgrund des stechenden Gefühls von Rose Bengal ist dies möglicherweise nur für ganz bestimmte Zwecke erforderlich.
Die Intensität der Vitalfärbung kann optimiert werden (z. B. für die Vitalfärbung der Lid Wiper Epitheliopathie der marginalen Bindehaut), indem 2% Fluorescein mit 1% Lissamingrün gemischt werden und ein Tropfen (40 µl) zweimal im Abstand von 5 Minuten aufgetragen wird. Die Färbung kann dann eine Minute nach dem zweiten Tropfen analysiert werden.
Da Fluorescein als intensivere Färbung für die Hornhaut beschrieben wird, während Lissamingrün für die Bindehaut bevorzugt wird, sollte die beschriebene Kombination beider Färbungen optimale Ergebnisse für die Vitalfärbung beider Epithelien ergeben.
Eine potenzielle Herausforderung kann auftreten, da die Beleuchtung möglicherweise umgeschaltet werden muss, da Fluorescein am besten mit blauem Licht wahrgenommen wird, während Lissamingrün am besten mit normalem weißem Licht wahrgenommen wird.
Schleimhaut- Status - Bindehaut- Stroma
LId- Parallele COnjunctivale Falten (LIPCOF) beim chronischen Trockenen Auge
Eine schematische Zeichnung eines Auges mit mehreren Lid Parallelen Falten (LIPCOF, durch Pfeile gekennzeichnet). Sie liegen über dem hinteren Lidrand innerhalb des Tränenmeniskus (blaue Pfeile). (Die Lidränder sind leicht nach außen gedreht, um die hintere Lidkante mit dem Tränenmeniskus darzustellen)
Lid- Parallele Conjunctivale Falten, meist abgekürzt als LIPCOF sind ein wichtiges Zeichen eines chronischen entzündlichen Trockenen Auges.
Sie zeigen eine Auflockerung der Bindehautstruktur (Conjunctivochalasis) an. Die Auflockerung entsteht durch erhöhte Reibung verbunden mit Gewebe-auflösende Enzymen (meist MMP9) im Rahmen der Entzündung beim chronischen Trockenen Auge.
Diese Auflockerung wird als Conjunctivochalasis bezeichnet. Dies leitet sich ab vom griechischen Wort χάλασις , "chalasis" für “Lockerung”. Conjunctivochalasis bezeichnet eine allgemeine Lockerung der Bindehaut, während LIPCOF Falten eine besondere Form der Bildung von Falten aus chalatischem Konjunktivagewebe auf der hinteren Lidkante sind.
LIPCOF Falten wurden entdeckt und benannt von Frank Schirra während seiner Promotionsarbeit bei Prof. Höh in Saarbrücken Mitte der 1990erJahre. Sie bilden sich parallel zum Lidrand und sind vor allem in temporaler Position gut sichtbar (siehe Abbildung).
Mit zunehmender Beschädigung des Bindehautgewebes nimmt die Anzahl und Grösse der Falten zu. Die LIPCOF Falten können sich dabei übereinander lagern und aus dem Tränenmeniskus herausragen (siehe Abbildung).
Die Schweregrad Einteilung von LIPCOF - und damit des Trockenen Auges - erfolgt nach der Höhe der Falten auf dem temporalen Unterlid Rand.
Erhöhte Reibung begünstigt LIPCOF Falten
Die Entstehung der LIPCOF Bindehautfalten wird begünstigt durch erhöhte Reibung. Diese entsteht aufgrund der verminderten Schmierungs-Wirkung des gestörten Tränenfilms.
Erhöhte Reibung wirkt sich aus bei Bewegungen des Buibus bei Blickbewegungen und besonders beim häufigen Lidschlag (siehe animierte Abbildung).
Dies führt zu einer Entzündungsreaktion der Bindehaut, die zuerst subklinischen, also unsichtbar ist. Es werden aber bereits Entzündungsmediatoren inklusive Gewebe-auflösende Proteinasen freigesetzt, die zusammen mit der erhöhten Reibung zu LIPCOF-Falten führen
Tränenfilmmangel => verminderte Schmierung => erhöhte Reibung => Beschädigung und Aktivierung der Epithelzellen
erhöhte Aktivierung von Proteasen => Beschädigung des Bindehautstromas => Konjunktivochalasis
Bindehautentzündung + erhöhte Reibung = LIPCOF - Bindehautfalten
Der Lidschlag schiebt die lockere Bindehaut zu LIPCOF Falten auf
LIPCOF Falten sind, wie die Abkürzung besagt, eine sehr spezifische Form der Bindehaut-Auflockerung - sie sind ' Lid Parallel Conjunctivale Falten'.
Das beschädigte und aufgelockerte (´chalatische´) Bindehautgewebe wird bei jedem Lidschlag durch die Bewegungen der hinteren Lidkante auf dem Bulbus bewegt und dabei hin und her geschoben.
Der Mechanismus der LIPCOF Bildung ist ähnlich einem Schneepflug, der den losen Schnee vor sich her schiebt. Dadurch bilden sich allmählich Bindehautfalten auf dem Lidrand. Auf dem unteren Lidrand sind sie, aufgrund der Orientierung der Lider, besser sichtbar als oben.
Da konjunktivale LIPCOF-Falten eine typische Folge einer Conjunctivochalasis sind, werden diese beiden Begriffe gelegentlich als Synonyme verwendet, was vielleicht nicht ganz richtig ist.
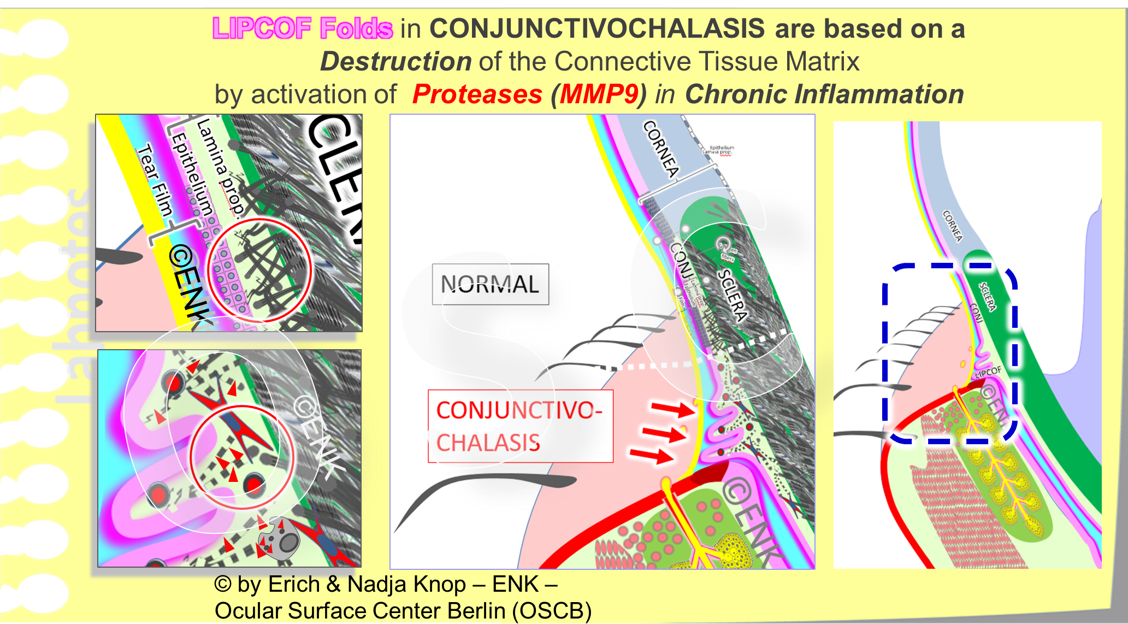
Lid-Parallele Conjunctivale Falten (LIPCOF) treten auf, wenn das strukturgebende Kollagengeflecht des Bindegewebes (Lamina propria) der Bindehaut durch Proteinasen abgebaut wird, hauptsächlich Matrix-Metalloproteinase 9 (MMP9). Dies dient dazu Platz im Gewebe zu schaffen für die Entzündungszellen, die beim chronisch entzündlichen Trockenen Auge aus den Gefässen in das Gewebe einwandern. Diese Entzündung muss nicht klinisch sichtbar sein, da auch bereits bei subklinischer Entzündung Matrix Metalloproteinasen aktiviert werden. Die Lockerung der Bindehaut wird als "Conjunctivochalasis" bezeichnet. Das lockere Gewebe wird dann durch die relativ scharfe hintere Lidkante ´aufgeschaufelt´ und auf dem Lidrand aufgefaltet. Der Einfachheit halber wird hier (Abb. links) direkt neben der ´Conjunctivochalasis´ eine Zone mit ´Normal´er -Kollagenstruktur angezeigt. Es ist jedoch davon auszugehen, dass die gesamte Bindehaut von dieser Beschädigung bei chronischem Trockenen Auge relativ homogen betroffen ist.
LIPCOF können zur Einteilung des Schweregrades für das Trockene Auge genutzt werden
Je nach Fortschreiten des Trockenen Auges steigt auch der Grad der konjunktivalen Schädigung und die Anzahl und Größe der LIPCOF-Falten. Zuerst gibt es nur eine kleine Falte, die kaum nachweisbar ist. Später nimmt die Größe der Falten zu. Sie entstehen im Bereich der hinteren Lidkante und liegen auf dem Epithel der sogenannten “mucocutaneous junction” (Haut-Schleimhaut-Grenze des Lides), d.h. am Boden des Tränenmeniskus.
In fortgeschrittenen Stadien werden mehrere Falten übereinander gelegt und ragen aus dem Tränenmeniskus in die Luft. Die Trocknung des Gewebes führt zu Reizung und Irritationsgefühl bis zu Schmerz.
Da der Grad der LIPCOF-Falten mit zunehmender Schwere der Erkrankung zunimmt sind die Falten ein wichtiges klinisches Zeichen. Der Ausprägungsgrad der LIPCOF-Falten wird verwendet zur Klassifizierungen für den Schweregrad des Trockenen Auges.
LIPCOF - Schweregradeinteilung (nach Schirra, Höh)
Die Einteilung erfolgt in 4 Stufen:
(Stufe 0: keine LIPCOF Falten = Normal)
Stufe 1: kleine Falte innerhalb des Tränenmeniskus
Stufe 2: grosse Falte bis zur Höhe des Meniskus
Stufe 3: grosse Falte mit Sub-Falten über Meniskushöhe
Stufe 4: grosse Falte, die über den inneren Lidrand reicht
LIPCOF Falten können eine erhöhte Tränenmenge (TMH) vortäuschen
Ausgeprägte LIPCOF Falten im Tränenmeniskus können die Oberkante des Meniskus nach oben verschieben und so eine erhöhte Tränenmenge auf dem Auge vortäuschen.
LIPCOF-Falten liegen am hinteren Lidrand und werden in fortgeschrittenen Stadien übereinandergelegt. Die niedrigste, d.h. erste Falte ist in der Regel die größte und ragt in vorderer Richtung am weitesten hervor, wohingegen die folgenden Falten mit jeder Falte kleiner werden.
Dabei liegen LIPCOF im Tränenmeniskus und füllen ihn zunehmend und drücken so das obere Ende (Höhe) des Meniskus nach oben.
Die sichtbare Tränen-Meniskushöhe (TMH) wird gemessen oder semiquantitativ eingeschätzt, um einen Eindruck von der Meniskusfüllung und damit vom Volumen der präokularen Tränenmenge zu erhalten.
Daher kann das Vorliegen von extensivem LIPCOF zu einer Fehldiagnose führen, d.h. fälschlicherweise wird ein zu hohes Tränenvolumen angenommen. Diese Beobachtungen wurden von Pult und Pult veröffentlicht.
Diagnose von Entzündungsfaktoren
MMP9 (Matrix-Metalloproteinase 9) ist ein Gewebe-abbauendes Enzym
Entzündung beim chronischen Trockenen Auges kann typischerweise eine fortschreitende Schädigung des Gewebes hervorrufen.
Die Grundstruktur der Konjunktiva besteht aus dem luminalen Epithel und dem darunter liegenden Geflecht aus Kollagenfasern im Bindegewebe der Lamina propria. In den Spalten zwischen den Fasern befinden sich Stromazellen und Abwehrzellen des angeborenen und spezifischen Immunsystems zusammen mit umgehenden Strukturen wie Blutgefäßen (links in der Mitte), Lymphgefäßen und Nervenfasern (schwache gelbe Linien). Das Enzym MMP9 spaltet die langen Kollagenfasern in Fragmente und beschädigt so die strukturelle Basis des Gewebes. Der biologische Sinn liegt darin, mehr Platz für die eigentlich schützenden ´Entzündungszellen´ zu schaffen. Probleme treten dann auf, wenn die Entzündung chronisch wird und somit alle Versuche einer endgültigen, geordneten Reparatur des Gewebes untergräbt. Dies führt zu einer zunehmenden Beschädigung und damit zu einer Gewebelockerung der Bindehaut, die als Conjunctivochalasis bezeichnet wird
Auch wenn eine sichtbare Beschädigung noch nicht stattgefunden hat, können dennoch bereits erhöhte Mengen gewebeabbauender Enzyme vorliegen und die Augenoberfläche schädigen.
Dies sind meist Matrix-Metalloproteinasen (MMP). Beim Trockenen Auge ist vor allem der Subtyp Matrix-Metalloproteinase 9 (MMP9) wichtig.
Für diesen wichtigen Krankheitsfaktor, der das Gewebe der Augenoberfläche abbaut, ist auch ein klinischer Test verfügbar.
Die Beschädigung der Bindegewebs-Struktur der Konjunktiva durch MMP9 wird schematisch in der nachfolgenden Abbildung gezeigt.
Das gewebeauflösende Enzym MMP9 wird ausgeschüttet als Teil einer eigentlich schützenden Entzündungsantwort. So soll Platz geschaffen werden für eine effektive Entzündung zur Ausschaltung eines auftretenden Reizes.
Durch die chronische Reizung beim Trockenen Auge wird jedoch andauernd und massiv MMP-9 aktiviert und es kann keine normale Reparatur bzw. Heilung erfolgen.
Matrix Metalloproteinasen sind wichtige Faktoren einer Entzündung
Gewebe-abbauende Enzyme wie Matrix-Metallo-Proteinasen (MMP) sind wichtige Entzündungsmediatoren, die Proteine spalten.
Sie werden produziert und aktiviert durch Einfluss von Entzündungsmediatoren wie Entzündungslipide, z.B. Eicosanoide, Histamin und Entzündungszytokine, die durch den Einfluss eines pathogenen Reizes auf das Gewebe entstehen.
Der pathogene Reiz, der als “Gefahr” wahrgenommen wird, kommt typischerweise von aussen in Form von z.B. erhöhter mechanischer Reibung, Hyperosmolarität, einer Infektion oder anderer Schäden. Mechanische Reibung aufgrund geringer Schmierung und Hyperosmolarität aufgrund erhöhter Wasserverdunstung treten typischerweise bei der Erkrankung des trockenen Auges auf und treffen die Epithelzellen, die die ersten Produzenten von entzündungsvermittelnden Stoffen wie Zytokinen zu sein scheinen.
Matrix Metalloproteinasen lösen das Kollagengerüst des Gewebes auf
Eine Entzündungsreaktion ist eine grundlegende Schutzantwort für Gewebe:
durch Vermehrung von Adhäsionsmolekülen, z.B. auf vaskuläre Endothelzellen, wandern mehr Abwehrzellen in das Gewebe ein
Abwehrzellen sind notwendig für eine effektive Ausschaltung jedes zellaktivierenden Reizes.
Die effektivste Schutzreaktion des Körpers ist eine Entzündung - daher werden Abwehrzellen auch oft vereinfacht als Entzündungszellen bezeichnet.
die große Menge an ankommenden Abwehr-Zellen benötigt aber mehr Platz in den engen Gewebespalten der Kollagenfasermatrix, um ihre Arbeit so gut wie möglich zu erledigen.
Lid-Parallele Conjunctivale Falten (LIPCOF) treten auf, wenn das strukturelle Kollagengeflecht des Bindegewebes (Lamina propria) in der Konjunktiva durch Proteinasen abgebaut wird, hauptsächlich Matrix-Metalloproteinase 9 (MMP9). Die Lockerung der Bindehaut wird als "Conjunctivochalasis" bezeichnet. MMP9 wird zunehmend während des chronischen Entzündungsprozesses beim Trockenen Auge aktiviert. Die lockere Bindehaut wird dann durch die relativ scharfe hintere Lidkante ´aufgeschaufelt´ und auf den hinteren Lidrand gefaltet. Hier schematisch direkt neben der Conjunctivochalasis eine Zone mit ´Normal´ er Kollagenstruktur angezeigt. Es ist jedoch davon auszugehen, dass die gesamte Bindehaut von dieser Zerstörung bei chronischer trockener Augenerkrankung relativ homogen betroffen ist.
Daher werden Proteasen aktiviert, die die Matrix des stromalen Bindegewebes der Augenoberfläche abbauen können und so Platz im Gewebe schaffen.
Das Bindegewebe-Gerüst (Matrix) besteht hauptsächlich aus Proteinen, überwiegend aus Kollagenfasern (wie in der Abbildung dargestellt). Sie bilden das strukturelle Geflecht, in dem sich die Stromazellen und Stützstrukturen, Abwehrzellen, Blut- und Lymphgefäße, Nerven usw. aufhalten.
An der Augenoberfläche, beim chronischen Trockenen Auge, ist vor allem die Matrix-Metalloproteinase MMP9 von Bedeutung, die z. B. von Steven PFLUGFELDERs Gruppe, von MELLER und TSENG und von anderen gezeigt wird.
LIPCOF Falten der Bindehaut sind ein Zeichen für eine chronische Entzündung - auch wenn diese noch subklinisch abläuft
Die chronische Aktivierung von Proteasen (hauptsächlich MMP9), im Rahmen der chronischen Entzündung beim Trockenen Auge kommt bereits bei einer chronische subklinischen Entzündung vor, ohne die Kardinalzeichen einer Entzündung, und ist daher für den Arzt nicht einfach erkennbar.
Die Entzündung beim Trockenen Auge ist zuerst subklinisch und erst klinisch erkennbar wenn eine Rötung oder Schwellung der Bindehaut oder konjunktivalen LIPCOF-Falten vorliegen.
LIPCOF Falten sind also ein erstes Zeichen einer chronischen Entzündung beim Trockenen Auge. Allerdings ist dann auch bereits eine Beschädigung des Gewebes eingetreten.
Für eine frühere Erkennung einer Entzündung, die eine Indikation sein kann für eine frühere und damit effektivere Therapie, ggf. mit anti-entzündlichen Medikamenten, sind biochemisch-immunologische Tests notwendig. Dies ist möglich über einen klinischen Test für den wichtigen Entzündungsmediator MMP9.
Der MMP9-Protein Test identifiziert sub-klinische Entzündung und kann ein vorbeugender Ansatz für das Trockene Augen sein
Ein geeigneter Test zur Bestimmung erhöhter Spiegel des proteinzerstörenden Enzyms Matrix-Metalloproteinase 9 (MMP9) ist verfügbar. Durch eine Immunreaktion wird angezeigt, ob der MMP9-Spiegel über dem normalen Bereich liegt. Der MMP9-Test kann somit einen chronischen gewebezerstörenden Entzündungsprozesses anzeigen, der eine therapeutische Intervention erfordert, selbst wenn klinische Anzeichen einer Gewebezerstörung noch nicht aufgetreten sind. Der MMP9-Test bietet daher möglicherweise einen neuen präventiven Ansatz für die Behandlung von Krankheiten des trockenen Auges.
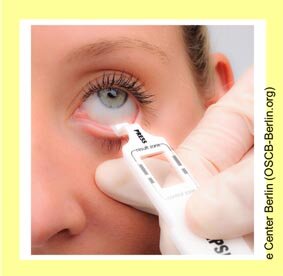
Es ist ein diagnostischer Schnell-Test verfügbar, bei dem eine erhöhte MMP9 Konzentration festgestellt werden kann.
Dies ist ein einfach durchzuführender Test, der direkt am Patienten durchgeführt werden kann. Er erfordert nur das Sammeln von einigen Tränen und etwas oberflächlichem Zellmaterial vom Bindehautgewebe im unteren Fornix.
Der MMP9-Test arbeitet mit einer Immunreaktion, die durch das Auftreten einer Farbreaktion sichtbar wird, wenn der Test positiv ist - ähnlich wie bei einem Schwangerschaftstest.
Dieser praktische neue Test erlaubt vermutlich den Nachweis erhöhter MMP9-Spiegel, und damit einer Entzündung, bevor schädliche klinische Symptome auftreten, wie eine Lockerung des Bindehautgewebes mit LIPCOF Falten.
Ein solcher klinischer MMP9-Test könnte daher eine Chance für einen präventiven Aspekt beim Trockenen Auge bieten.
Status der Meibom Drüse - MEIBOGRAPHIE
Das Interesse an den Meibom Drüsen hat stark zugenommen, nachdem bekannt wurde, dass ein Mangel an Tränenfilm-Lipid aufgrund einer hauptsächlich obstruktiven Dysfunktion der Meibom Drüsen die Hauptursache für die Erkrankung des trockenen Auges darstellt.
Dies mag für viele eine Überraschung sein, da der Begriff "Trockenes Auge" auf einen primären Wassermangel hinzudeuten scheint. Viele Trockene-Augen-Spezialisten haben jedoch seit langem erkannt, dass Veränderungen der Lipidphase häufig auftreten, wie z. B. durch eine Schaumbildung auf dem Tränenfilm und dem Lidrand. Der Schaum entsteht durch die Verseifung von Tränenfilmlipiden oder lipidhaltigen Verkrustungen am Lidrand und am den Boden von Wimpern.
Die Meibomdrüsen in den Augenlidern sind klinisch nur schwer zu beobachten
Der Spezialist für die Augenoberfläche ist, im Vergleich zu vielen anderen medizinischen Gebieten, im Allgemeinen dadurch gesegnet, dass die meisten anatomischen Strukturen und pathologischen Ereignisse in seinem Interesse leicht erkennbar sind.
In dieser Hinsicht stellen die Meibom Drüsen sicherlich eine unerwartete Herausforderung dar, denn sie sind verborgen in der Tiefe der der Augenlider.
Von vorne sind die Meibomdrüsen durch die vordere Lidlamelle mit der Haut und den Lidmuskeln nicht zu sehen.
Von der Rückseite der Lider durch die relativ transparente Bindehaut sind die einzelnen Meibom Drüsen als weißliche Streifen erkennbar. Allerdings zeigen sich dabei kaum Details (siehe Abbildung B).
Meibographie war bisher nur in der Forschung verbreitet
Eine erste Welle des Interesses an den Meibom-Drüsen war in den 1980er Jahren nach der Entdeckung der "Meibomian Gland Dysfunction, MGD” (dt.: Meibomdrüsen Dysfunktion, MDD) durch KORB und HENRIQUEZ. Danach führte eine Gruppe um einen Mann namens James JESTER frühe Experimente durch, die sich auf die Hyperkeratinisierung des Drüsenepithels konzentrierten. Sie stellten die Drüsen dar mit Durchleuchtung der Lider mit Infrarotlicht von der vorderen Hautseite aus - die Beobachtung erfolgte von der Rückseite durch die Bindehaut.
wenn eine solche Visualisierung der Meibomdrüsen nur beobachtet wird, wird sie als 'Meiboskopie' bezeichnet.
wenn das Bild aufgenommen wird, wird sie als 'Meibographie' bezeichnet.
KONTAKTLOSE MEIBOGRAFIE MIT INFRAROT-BELEUCHTUNG UND CCD-KAMERA HAT DIE KLINISCHE BEOBACHTUNG DER MEIBOMISCHEN DRÜSE GROSS REVOLUTIONIERT
Eine neuartige Technik der MEIBOGRAPHIE wurde von entwickelt von Reiko ARITA und Kollegen in Tokio. Diese Methode wird Non-Contact Infrared Meibography (dt.: Kontaktfreie Infrarot Meibographie) genannt und wurde in einer wegweisenden Arbeit im Jahr 2008 beschrieben. Diese Technik:
es wird Infrarotlicht verwendet, da dies den Lipidgehalt der Meibom Drüsen besonders gut zeigt
auch hier werden die Drüsen von der Bindehautseite beobachtet, was sicherlich sinnvoll ist,
mit einer Infrarot-Digitalkamera, die an einer Spaltlampe angebracht ist.
Diese Apparatur wurde von Topcon Japan Inc. maßgeschneidert und stand später allen interessierten Klinikern als kommerzielles Paket zur Verfügung.
Meibographie zeigt die Struktur des Drüsengewebes an der Spaltlampe
Im Gegensatz zu früheren Meibographietechniken erfolgt die Beleuchtung von der gleichen Seite wie die Beobachtung, d.h. von der Seite der Bindehaut. Da relativ mehr Lichtintensität die Meibom Drüsen erreicht, ist der Kontrast des Bildes und damit die Klarheit besser als mit früheren Techniken.
ARITA und Kollegen haben inzwischen eine Forschungsgruppe namens " Lid and Meibomian Gland Working Group " (LIME , http://www.lime.jp/en/) gegründet, die auf dem Gebiet der Meibom Drüsen viele Fortschritte erzielt hat. Dysfunktion und organisieren auch jährliche internationale Forschungstreffen.
Der Begriff ´kontaktfrei´ in der Beschreibung der Methode ist möglicherweise etwas irreführend. Das Augenlid muss zur Beobachtung natürlich berührt und manipuliert werden, um es von der Innenseite aus zu betrachten. Allerdings erfolgen Beleuchtung und Beobachtung kontaktfrei.
Zur Beobachtung muss das leichter zugängliche Unterlid leicht evertiert werden und das schwieriger zugängliche Oberlid muss ektropioniert werden.
Die Kontaktfreie Infrarot Meibographie stellt einen grossen Fortschritt in der Diagnostik des Trockenen Auges dar. So können, direkt am Patienten in der Praxis, Untersuchungen über den Zustand der funktionell äusserst wichtigen Meibomdrüsen durchgeführt werden, die früher eine Biopsie erfordert hätten
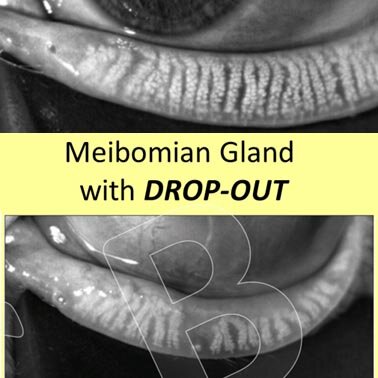
Die Meibographie zeigt die Struktur und Orientierung der Drüsen, je nach Gerät, in unterschiedlicher Qualität und erlauben vor allem Ausfälle des Drüsengewebes (engl.: Gland Drop-outs) zu erkennen.
Ausfälle beschreiben das Verschwinden von Teilen des Drüsengewebes im Infrarotbild. Dies deutet auf ein Verschwinden von funktionellem Drüsengewebe hin.
Diese Annahme erscheint richtig, da der Grad des Drüsenausfalls im Allgemeinen mit der Drüsenfunktion und dem Grad der Erkrankung des trockenen Auges korreliert. Ausserdem wurde auch durch lichtmikroskopische histologische Befunde eine Drüsenzerstörung mit Verschwinden von Drüsengewebe bestätigt.
Daher ist die Meibographie zu einem wertvollen neuen diagnostischen Parameter in der Diagnostik des trockenen Auges geworden. Der Drüsenausfall beginnt typischerweise am Ende der Meibomdrüsen, d.h. an dem Teil, der von der Mündung am hinteren Lidrand entfernt ist.
Offensichtlich unterschiedliche pathogenetische Einflussfaktoren können Drüsenstörungen verursachen, wie im Kapitel über die Meibomdrüsen Dysfunktion (MDD) erörtert wird. Beim Tragen von Kontaktlinsen, unabhängig vom Linsentyp, nehmen die Ausfälle drastisch zu. Auch bei entzündlichen Bindehautallergien treten Drüsenausfälle auf.
Für den klinischen Einsatz stehen Bewertungsskalen zur Verfügung:
Für Gland-Drop-Out stehen mehrere semiquantitative Bewertungsskalen zur Verfügung, die grundsätzlich alle relative Mengen des Ausfalls bewerten. Derzeit gibt es noch keine Software, die vollautomatisch den Grad des Drüsenausfalls ermitteln kann.
Bei der Meibomdrüsen Dysfunktion wir das Drüsengewebe im Augenlid zerstört
Lichtmikroskopische Darstellung einer geschädigten Meibomdrüse (rechts) im Vergleich mit einer normalen Drüse (links)
In der lichtmikroskopischen Analyse sind die Schäden der Meibomdrüse durch Verstopfung erkennbar:
wenn die Drüsenöffnung dauerhaft verstopft ist (kleine rote Kreisline in Abbildung)
führt das angesammelte Sekret zur Druckerhöhung in der Drüse mit Erweiterung der Gänge
die Öl-bildenden Zellen befinden sich in rundlichen Haufen (Endstücke, Azini) und werden zerstört
schliesslich bilden sich die Ölbildenden Zellen ganz zurück
(grosse rote Kreisline in Abbildung)
Diese Veränderungen entsprechen etwa dem Verlust an Drüsengewebe, der in der Meibographie sichtbar ist.
Topographer-Systeme sind in der Regel weiter fortgeschritten. Sie bieten in der Regel fortschrittlichere Beleuchtungs- und Visualisierungstechniken und eine bessere Bildqualität sowie Messungen und eine strukturierte Dokumentation, die den täglichen Effektiver und angenehmer gestalten können.
Höchste Bildqualität bei der Meibographie ist möglich… aber sie benötigt eine spezielle Beleuchtungs- und Auswertungstechnik
Ein häufiges Problem bei der Darstellung der Meibomdrüsen im Augenlid des Patienten, direkt in der Praxis des Arztes, beruht darauf, dass Augenoberfläche eine natürliches ´Feuchtgebiet´ ist - eine Schleimhaut. Da sie eine feuchte Oberfläche hat, werden bei der Beleuchtung viele störende Reflexionen produziert.
Störende Reflexionen verschiedenen treten typischerweise auf den meisten Meibographie Bildern auf. Es erfordert einen gewissen Grad von Erfahrung des Untersuchers die Reflexionen möglichst gering zu halten. Nur so kann ein aussagekräftiges Foto für die klinische Verlaufs-Dokumentation hergestellt werden.
Andererseits erlaubt es eine Foto-Dokumentation mit perfektem Kontrast und Auflösung, die Meibomdrüsen so darzustellen, als wären sie freiliegend und nicht bedeckt von dem darüberliegenden Gewebe der Lidplatte und der Augenbindehaut. Dadurch ist die Struktur der Drüsen unmittelbar erkennbar für den Arzt … und auch für den Patienten.
Man darf annehmen, dass diese realistische Darstellung der Meibomdrüsen auch dem Patienten erlaubt unmittelbar zu verstehen, wie der Zustand ´seiner´ Meibomdrüsen mit den Beschwerden des Trockenen Auges zusammenhängt. Die erlaubt Einsicht, wie wichtig therapeutische Massnahmen sind, z.B. eine konsequente heimische Physikalische Lidrand Therapie.
Die perfekte und störungsfreie Darstellung eines schwierigen Objekts wie der Meibomdrüsen, erfordert ein anspruchsvolles System für die Beleuchtung und für die elektronische Bildverarbeitung. Aktuell gibt es nur einen Gerätetyp, der Meibomdrüsen Bilder von bisher unbekannter Klarheit und Präzision in nahezu histologischer Auflösung erzeugt - das Lipiview und das Lipiscan (Fa. TearScience Inc.).
Als (leichter) Nachteil ist anzumerken, dass diese Maschinen so spezialisiert sind, dass sie nur für die Meibographie (Lipiscan) oder für Meibographie und Lipidschicht-Interferometrie optimiert sind - sie können also ein Mehrzweck-Arbeitspferd wie einen Topographen nicht vollständig ersetzen.
Fortschrittliche Beleuchtungstechniken ermöglichen die Abbildung der Meibomschen Drüsen in beispielloser Klarheit. Dadurch kann die genaue Struktur normaler Meibom-Drüsen und genaue Information über deren Änderung beim Drüsenabbruch erhalten werden. Bilder: Mit freundlicher Genehmigung von TearScience Inc.